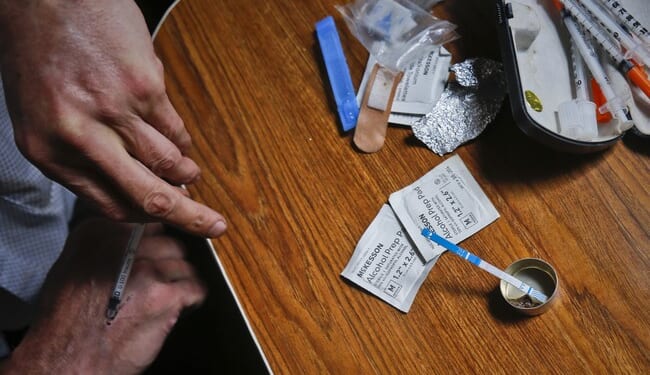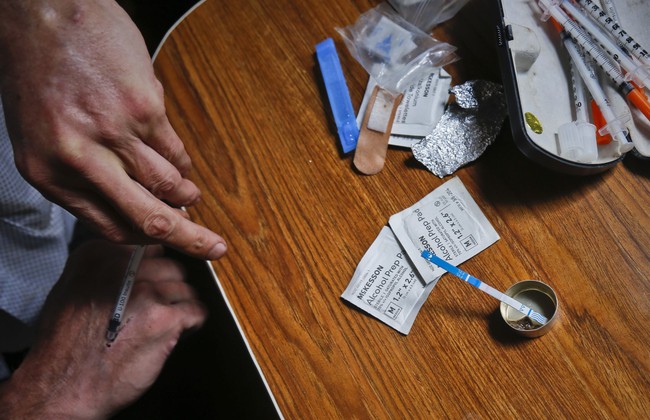
America is facing overlapping epidemics of addiction, depression, anxiety, trauma, and despair. Conventional psychiatric and addiction treatments have helped many people and remain important tools in medicine. Yet millions continue to struggle despite years of medications, counseling, detoxification attempts, and repeated efforts at recovery.
For too many patients and families, the search for healing has felt painfully hopeless. This is reinforced by the fact that traditional substance abuse programs have a success rate of less than 10%.
That is one reason why growing interest in compounds such as Ibogaine and other psychedelic-assisted therapies has generated so much hope among clinicians, researchers, and patients alike. Increasingly, these agents are being viewed not as fringe ideas, but as potentially important breakthroughs in how we understand healing, neuroplasticity, trauma, and recovery.
What makes Ibogaine particularly compelling is that many individuals describe not merely a reduction in cravings or symptoms, but a profound shift in perspective—an ability to step outside destructive emotional and behavioral loops that may have dominated their lives for years. In fact, many patents report that that it felt like Ibogaine “reset their brain” to a point in time before they ever used drugs.
For some people struggling with addiction, trauma, or severe depression, that possibility can be life-changing.
Emerging research into psychedelic-assisted therapies more broadly is also beginning to suggest that these compounds may help the brain temporarily become more flexible, adaptive, emotionally open, and receptive to change. In a society where so many people feel emotionally trapped, disconnected, or numb, that possibility deserves serious and hopeful exploration.
At the same time, enthusiasm should be matched with responsibility.
These are powerful agents, not casual wellness products. In our view, therapies involving Ibogaine or related compounds should be administered within carefully designed, highly individualized protocols overseen by trained professionals.
That individualized approach may ultimately become one of the greatest strengths of this emerging field.
Mental health conditions and addiction are rarely caused by one factor alone. Biology, trauma, inflammation, stress, sleep disruption, nutritional depletion, social isolation, emotional pain, and spiritual disconnection can all interact in ways that profoundly shape mental well-being. Effective treatment should therefore address the whole person rather than focusing narrowly on symptoms.
This is where the future of mental health care may be headed: toward integrative models that combine innovative therapies with comprehensive support for mind, body, and spirit.
In practice, that means patients should receive careful medical and psychological screening, appropriate supervision, and long-term integration support. It also means recognizing the potential importance of complementary approaches such as nutritional optimization, restorative sleep, physical activity, mindfulness practices, trauma-informed therapy, community support, and spiritual grounding.
The goal should not simply be symptom suppression.
The goal should be transformation.
What is perhaps most encouraging about this moment is that medicine may finally be beginning to embrace a more complete understanding of healing itself. Human beings are not merely collections of symptoms or neurochemical pathways. People need meaning, connection, hope, resilience, and purpose. Treatments that help unlock those capacities—when administered safely and thoughtfully—could represent a major evolution in mental health care.
Of course, continued research is essential. Safety standards must remain rigorous, especially with compounds such as Ibogaine, which can carry significant medical risks if improperly administered. Scientific integrity and responsible clinical oversight are non-negotiable.
But optimism is justified.
Throughout medical history, some of the most important advances began as unconventional ideas that challenged existing assumptions. Today, many patients, clinicians, and researchers believe we may be standing at the beginning of a similarly important shift—one that moves mental health care beyond symptom management alone and toward deeper healing and recovery.
People battling addiction, depression, trauma, and anxiety are not simply seeking relief from pain. They are searching for clarity, reconnection, emotional freedom, and a renewed sense of possibility.
Treatments like Ibogaine may not be the entire answer. But when integrated into individualized, professionally guided, and holistic models of care, they may ultimately help many people reclaim lives they feared had been permanently lost.
That possibility should inspire both hope and serious attention.
Editor’s Note: Do you enjoy PJ Media’s conservative reporting that takes on the radical Left and woke media? Support our work so that we can continue to bring you the truth.
Join PJ Media VIP and use promo code FIGHT to receive 60% off your membership.